Dental implants have transformed modern dentistry, offering a robust and natural solution for individuals dealing with missing teeth. This ultimate guide aims to delve deeply into the world of dental implants, providing you with extensive knowledge ranging from the fundamental concepts to post-implant maintenance.
a. Definition and Evolution: Dental implants represent a remarkable advancement in dental technology, serving as artificial tooth roots crafted from biocompatible titanium. This material’s compatibility with the human body is pivotal, allowing for a seamless fusion with the jawbone, a process known as osseointegration. The evolution of dental implants traces back to the mid-20th century when Dr. Per-Ingvar Brånemark made the ground breaking discovery of osseointegration. This discovery laid the foundation for modern implantology, transforming the landscape of tooth replacement.
b. Components Explained: Dental implants comprise three essential components, each playing a crucial role in their functionality and longevity.
– Implant Fixture: This is the titanium post surgically embedded into the jawbone. Its design facilitates stability and mimics the root structure of natural teeth.
– Abutment: The abutment serves as a connector between the implant fixture and the prosthetic crown. It is typically a small, intermediary piece that plays a vital role in the final restoration.
– Prosthetic Crown: The crown, the visible part of the dental implant, is custom-made to replicate the size, shape, and colour of natural teeth. It is securely attached to the abutment, completing the implant and restoring both function and aesthetics.
Understanding the evolution and components of dental implants provides patients with a broader appreciation for the intricate science behind this transformative dental solution. This knowledge underscores the importance of choosing a qualified implant dentist who recognizes the significance of precision in implant placement in Leicester.

a. Aesthetics: Dental implants excel in providing a natural appearance due to their integration into the jawbone. Unlike removable dentures, implants fuse with the bone, preventing the sunken facial appearance that can result from missing teeth. The implant’s crown is meticulously crafted to match the colour, shape, and alignment of natural teeth, ensuring a seamless blend with the existing dentition.
b. Functionality: The restoration of biting and chewing capabilities is a significant benefit of dental implants. Unlike traditional alternatives, such as bridges, implants do not rely on adjacent teeth for support. This independence preserves the integrity of neighboring teeth and promotes long-term oral health. With dental implants, individuals can enjoy a varied diet without the limitations often associated with removable dentures.
c. Durability: The durability of dental implants is a testament to their long-term success. The key to this longevity lies in the process of osseointegration, where the implant fuses with the jawbone. This integration creates a sturdy foundation, mimicking the strength of natural tooth roots. Proper oral hygiene practices and regular dental check-ups contribute to the sustained durability of implants, making them a reliable and enduring solution for tooth replacement.
a. Consultation: The consultation phase is a collaborative effort between the patient and the implant dentist. It involves a thorough assessment of the patient’s oral health, medical history, and treatment goals. Advanced imaging technologies, such as 3D scans, aid in precise treatment planning. During this phase, patients can discuss any concerns, questions, or cosmetic preferences to ensure a personalised and satisfactory outcome.
b. Implant Placement Surgery: The surgical placement of dental implants is a carefully orchestrated procedure. The dentist makes an incision in the gum to access the jawbone, where the implant fixture is precisely positioned. Specialized drills are used to create a space for the implant, emphasizing accuracy to optimize osseointegration. The team employs sterile techniques, and post-operative care instructions are provided to minimize discomfort and support the healing process.
c. Osseointegration: Osseointegration is the cornerstone of successful implant integration. This biological process involves the fusion of the implant with the surrounding bone tissue. Patients are educated on the importance of following post-surgery care guidelines, including a restricted diet and meticulous oral hygiene practices. Regular follow-up appointments allow the dental team to monitor osseointegration progress and address any emerging concerns promptly.
d. Abutment and Crown Placement: Once osseointegration is confirmed, the abutment, a connector between the implant and the prosthetic crown, is attached. Impressions are taken to fabricate a customized crown that perfectly matches the patient’s natural teeth in colour, shape, and alignment. This final stage completes the restoration, providing a functional and aesthetically pleasing outcome.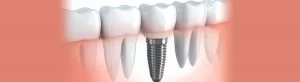
a. Oral Health Assessment: The journey toward dental implants begins with a comprehensive oral health assessment. Beyond assessing the presence of missing teeth, the dentist evaluates the overall health of the gums. Absence of periodontal disease is crucial, as healthy gums provide the necessary support for dental implants. Any existing dental issues, such as cavities or infections, are addressed before proceeding with the implant process. Regular dental cleanings and thorough examinations are essential in maintaining optimal oral health.
b. Jawbone Density: Sufficient jawbone density is a critical factor for the success of dental implants. The jawbone serves as the anchor for the implant fixture, and its density ensures stability and support. In cases where there’s insufficient bone, bone grafting procedures may be recommended to augment the bone volume. Advanced imaging technologies, including 3D cone-beam computed tomography (CBCT), aid in assessing the jawbone’s density and structure, guiding the implant planning process.
c. General Health Considerations: Beyond oral health, a patient’s overall health plays a significant role in determining implant eligibility. Conditions such as uncontrolled diabetes or autoimmune disorders may impact the body’s ability to heal and integrate the implant. A thorough medical history review ensures that the patient is in good overall health, setting the stage for a successful implant journey. Collaboration between the implant dentist and other healthcare providers may be necessary to address any systemic health concerns.
a. Endosteal Implants: These implants, placed directly into the jawbone, are the most common type. Their versatility makes them suitable for various restoration options, from single crowns to full arches. Endosteal implants offer stability and mimic the natural tooth root structure, providing a robust foundation for replacement teeth.
b. Subperiosteal Implants: Unlike endosteal implants, subperiosteal implants rest on the bone beneath the gum tissue. This type is often considered when there’s insufficient natural bone height for traditional implants. Customized to each patient’s unique jawbone shape, subperiosteal implants are placed on or above the jawbone, securing them in place. While less common than endosteal implants, they offer a viable alternative in specific clinical situations.
a. Cost Factors: The overall cost of dental implants is influenced by various factors, including the number of implants needed, the type of restoration (single crown, bridge, or full arch), and the materials used. High-quality materials, such as zirconia or titanium alloys, may contribute to a higher cost but often offer enhanced durability and aesthetics. Additionally, the need for supplementary procedures like bone grafting or sinus lifts can impact the total cost.
b. Fees and Financing: We offer financing options, allowing patients to manage the cost through instalment plans. Exploring these financial aspects during the initial consultation ensures transparency and helps patients plan for the investment in their oral health.
Oral Hygiene Practices: Maintaining impeccable oral hygiene is paramount for the long-term success of dental implants. Patients are educated on proper brushing techniques, using soft-bristle brushes to avoid damaging the crown or abutment. Flossing and interdental brushes help remove plaque from hard-to-reach areas. Antibacterial mouthwashes may be recommended to reduce the risk of infection. Regular dental check-ups and professional cleanings are essential, allowing the dental team to monitor the health of the implants and address any emerging issues promptly.
Follow-Up Appointments: Post-implant surgery, a series of follow-up appointments are scheduled to monitor the healing process. These appointments provide an opportunity to assess osseointegration, confirm the stability of the implant, and address any concerns or discomfort the patient may be experiencing. Adjustments to the bite or occlusion may be made during these appointments to ensure proper alignment and function of the implant-supported restoration.
Lifestyle Considerations: Patients are advised to be mindful of lifestyle habits that could impact implant success. Avoiding tobacco products is crucial, as smoking can hinder the healing process and increase the risk of complications. Additionally, maintaining a balanced diet rich in nutrients supports overall oral health and contributes to the longevity of dental implants.
a. Infection and Inflammation: While infection is rare due to the sterile nature of implant surgery, we like to educate patients to be able to recognizing signs of infection, such as persistent swelling or discomfort. Immediate reporting of such symptoms ensures prompt intervention. Anti-inflammatory medications and proper oral hygiene play pivotal roles in minimizing inflammation risks.
b. Implant Failure and Peri-implantitis: Implant failure is uncommon but can occur. Peri-implantitis, characterized by inflammation around the implant site, is a potential complication. Regular check-ups and adherence to aftercare instructions are crucial in detecting and addressing these issues early. Proper oral hygiene practices and, if necessary, professional cleaning help mitigate the risk of peri-implantitis.
c. Nerve Damage and Sinus Issues: While rare, nerve damage or sinus issues may occur, especially in upper jaw implant placements. Comprehensive preoperative assessments, including imaging studies, help identify potential complications. Experienced implant dentists take preventive measures to minimize these risks and ensure patient safety.
a. Credentials and Experience: We advise patients to research the credentials and experience of potential implant dentists. Board certifications, postgraduate education in implantology, and years of practical experience are indicative of a dentist’s expertise. Patient testimonials and case studies can provide insights into the dentist’s track record of successful implant placements.
b. Patient Reviews and Testimonials: Reading reviews from other patients provides valuable perspectives on the overall patient experience. Platforms such as online reviews and testimonials on the dentist’s website offer insights into the quality of care, communication, and satisfaction of previous implant recipients.
c. Consultation Process: The initial consultation is an opportune time for patients to assess the dentist’s communication style, willingness to address questions, and the thoroughness of the evaluation. A transparent discussion about treatment options, potential risks, and expected outcomes fosters trust and ensures patients make informed decisions about their implant journey.
a. Common Questions: Frequently asked questions cover a range of topics, from the initial consultation to post-implant care. Clear and detailed responses help alleviate concerns and empower patients to make informed decisions. Common questions include inquiries about the duration of the implant process, potential discomfort, and the expected appearance and functionality of the final restoration. See our blog “Dental implants common questions”
Back to blog
We are proud to help our valued patients to transform their smiles through a wide choice of general and cosmetic dental treatments.
Our TreatmentsWe ensure an exceptional patient journey – from start to finish.
learn moreDelivering life-changing smiles and ensuring excellent dental health.
learn moreDental implants and us – together we can recreate a naturally beautiful smile.
learn more